How to Sleep After a Hair Transplant: Positions, Pillows & Tips
The correct sleeping positions, pillow setups, and nighttime routines to protect your grafts during the critical first two weeks.

Sleep is one of the most common concerns patients raise after their hair transplant procedure. It is a valid concern. You spend roughly a third of your recovery time asleep, and during those hours you have limited control over your body's movements. Rolling onto the wrong side, pressing your face into a pillow, or allowing your head to drop flat can all put your newly transplanted grafts at risk during the critical first days of healing.
The good news is that with the right preparation, proper sleeping after a hair transplant is entirely manageable. Whether you had an FUE hair transplant or a no-shave FUE procedure, the sleeping guidelines are the same. This guide covers everything you need to know: the best sleeping positions, the most effective pillow setups, how to prevent unconscious rolling, and a clear timeline for when you can return to your normal sleeping habits.
Why Sleeping Position Matters After a Hair Transplant
During the first 7 to 10 days after surgery, the transplanted grafts are still establishing their connection to the blood supply in their new location. Until this process, called neovascularization, is complete, the grafts can be dislodged by direct pressure, friction, or shearing forces against a pillow or mattress surface.
Beyond graft protection, your sleeping position directly affects post-operative swelling. Lying flat allows fluid to accumulate in the forehead and around the eyes, which can be uncomfortable and alarming. Keeping the head elevated uses gravity to drain fluid away from the surgical area, significantly reducing the severity and duration of swelling.
There are two primary goals when sleeping after a hair transplant:
- Protect the grafts by ensuring nothing presses against or rubs the recipient area.
- Minimize swelling by keeping the head elevated above the heart.
The Best Sleeping Positions for Each Recovery Phase
Nights 1 Through 3: Elevated Back Sleeping Only
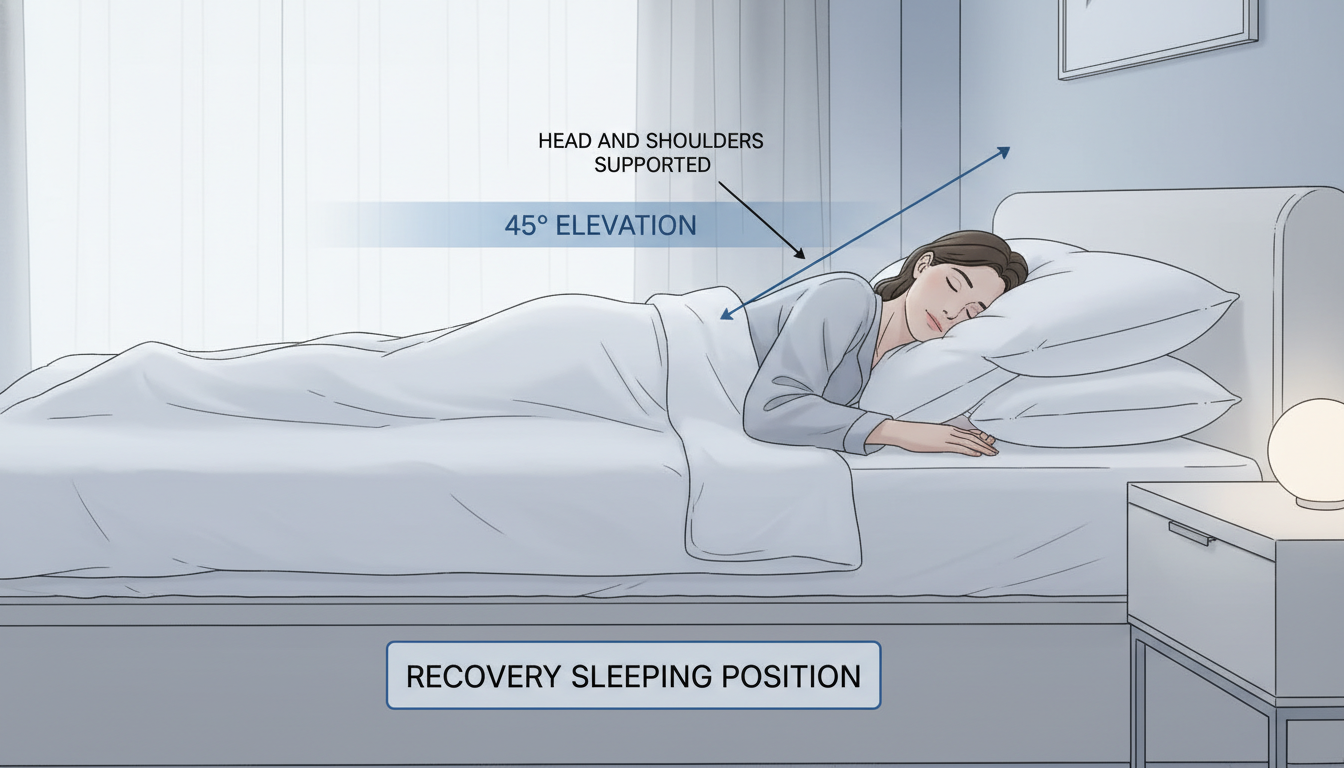
For the first three nights, you must sleep on your back with your head elevated to approximately 45 degrees. This is non-negotiable during the initial graft stabilization window. Side sleeping and stomach sleeping are both off limits because they create direct contact between the transplanted area and the pillow surface.
The 45-degree angle serves double duty: it keeps the grafts facing upward with no contact pressure, and it allows gravity to pull excess fluid downward, away from the forehead. Patients who maintain this elevated position consistently during the first three nights report significantly less swelling than those who slip down to a flatter angle during the night.
For detailed guidance on everything else happening during this window, including medications, swelling management, and diet, refer to our guide on post-operative care during the first 48 hours.
Nights 4 Through 7: Elevated Back Sleeping, Slightly Relaxed
After the first three days, you can reduce the elevation angle slightly to around 30 degrees. The grafts are becoming more stable, and the peak swelling period has passed. However, sleeping on your back remains the safest position. Side sleeping is still discouraged during this period because any contact with the recipient zone carries some risk.
Nights 8 Through 14: Gradual Transition
By the end of the first week, the grafts are significantly more anchored. Starting around night eight, most surgeons will allow patients to begin carefully sleeping on their side, provided the transplant was performed on the front and top of the scalp. If you had grafts placed on the sides of the head or in the crown area, you may need to continue back sleeping a bit longer. Check with your surgeon for personalized guidance.
You can begin reducing elevation further, sleeping at a gentle 15 to 20 degree incline or adding just one extra pillow. The key is to make changes gradually rather than suddenly returning to a completely flat position.
After Two Weeks: Return to Normal
By day 14, the grafts are considered fully secure in their recipient sites. At this point, you can return to sleeping in any position that is comfortable for you, including on your side or stomach, and on a flat surface without any extra elevation. The risk of graft dislodgement from sleeping is essentially zero after two weeks.
Pillow Setups That Work
The right pillow arrangement can make the difference between a restful night and hours of frustration. Here are four proven pillow setups that our patients have found effective during the first two weeks of recovery.
Option 1: The Recliner Chair
A recliner is widely considered the best sleeping surface for the first three to five nights after a hair transplant. It naturally positions your body at the correct angle, supports your back and neck, and makes it nearly impossible to roll onto your side during sleep. If you own a recliner or can borrow one, this is the setup we recommend most highly.
Adjust the recliner so your head is at roughly 45 degrees for the first three nights, then ease it back slightly to 30 degrees for nights four through seven. Place a soft blanket over the chair for comfort and keep a pillow behind your neck for additional support.
Option 2: The Wedge Pillow
A foam wedge pillow is the best bed-based solution. These triangular pillows are specifically designed to elevate the upper body while providing stable, consistent support. They come in various angles, typically ranging from 30 to 45 degrees, and they do not shift or flatten overnight the way stacked regular pillows can.
Place the wedge pillow at the head of your bed with its wide base flat on the mattress. Your entire upper body from the lower back to the head should rest on the incline. Add a thin, flat pillow on top for neck comfort. Wedge pillows are available at most home goods stores and online retailers, and they are worth the modest investment for the stability they provide.
Option 3: Stacked Bed Pillows
If you do not have access to a recliner or wedge pillow, you can create an effective elevated sleeping surface using three to four standard bed pillows. Stack them in a graduated arrangement: the bottom pillow flat, the next angled slightly higher, and the top pillow supporting your head and neck. The goal is to create a gradual slope rather than a sharp bend at the neck.
The downside of stacked pillows is that they tend to shift and flatten during the night, causing your head to gradually drop to a lower angle. To counteract this, place the pillow stack against the headboard for stability, and check your angle if you wake up during the night.
Option 4: The Travel Pillow Barrier
Regardless of which primary setup you use, adding a U-shaped travel pillow around your neck provides an extra layer of protection. The travel pillow acts as a physical barrier that prevents your head from turning too far to either side while you sleep. It also discourages you from unconsciously dropping your chin to your chest, which could bring the recipient area into contact with your chest or blankets.
The travel pillow is especially useful for patients who are naturally restless sleepers or who tend to move frequently during the night.
How to Prevent Rolling Over in Your Sleep
One of the most common fears patients express is that they will involuntarily roll onto their side or stomach during sleep and damage the grafts. This is an understandable concern, especially for habitual side and stomach sleepers. Here are several strategies that work:
The Pillow Fortress Method
Place a large pillow or body pillow on each side of your body, tucked firmly between your arm and torso. These side barriers create a physical obstacle that your body must overcome to roll, and in most cases, the resistance is enough to keep you in place or wake you up before you complete the roll.
The Towel Roll Technique
Roll two large bath towels into firm cylinders and place them under the fitted sheet on either side of where your torso rests. These hidden bumps create a subtle physical boundary that your body naturally stays within. This technique is less obtrusive than pillow barriers and allows more freedom of arm movement while still preventing full rolls.
The Backpack Method
Some patients find it helpful to wear a lightweight backpack filled with a pillow or soft item to bed. The bulge on the back makes it physically uncomfortable to roll onto the back of the head or to turn fully onto the stomach. This is particularly useful for dedicated stomach sleepers who struggle with other methods.

Special Considerations for Side Sleepers
If you are a dedicated side sleeper, the transition to back sleeping can be one of the most challenging aspects of recovery. Your body has spent years developing a preference for sleeping on its side, and breaking that pattern for even a few nights can feel difficult.
Here are specific tips for side sleepers:
- Practice before surgery. In the week leading up to your procedure, start sleeping on your back with an elevated pillow setup. This gives your body a few nights to begin adapting before the stakes are high.
- Use the recliner if possible. Recliners are the single best tool for side sleepers because the chair's structure physically prevents side rolling in a way that pillows alone cannot.
- Accept that sleep may be lighter. For the first few nights, you may not sleep as deeply or as long as usual. This is temporary and normal. Your body will adapt, and any sleep debt you accumulate will resolve quickly once you can return to your normal position.
- Use sleep aids cautiously. Some patients ask about taking melatonin or other sleep aids. Melatonin is generally safe and can help, but discuss it with your surgeon first. Avoid prescription sleep medications unless specifically approved, as they can cause deep sleep that makes you less responsive to your body's position.
Special Considerations for Stomach Sleepers
Stomach sleepers face the greatest challenge because their preferred position places the entire face and forehead directly into the pillow, which is the worst possible scenario for frontal hairline grafts. The backpack method described above is especially helpful for this group. Additionally, consider the following:
- The recliner is your best friend. It is essentially impossible to sleep on your stomach in a reclined chair.
- If you absolutely cannot use a recliner, the wedge pillow plus travel pillow combination provides the most resistance against face-down positioning.
- Set a gentle alarm for every two to three hours for the first two nights. This may sound extreme, but it ensures you can check your position and readjust if needed during the highest-risk period.
Dealing With Nighttime Discomfort
Discomfort during the first few nights is common but manageable. The primary sources of nighttime discomfort include:
Scalp Tightness and Soreness
The recipient and donor areas may feel tight, sore, or tender when you lie down because lying down changes the blood pressure distribution in the scalp. Taking your pain medication 30 minutes before you plan to sleep can help you fall asleep before any discomfort peaks. If you wake up sore during the night, take another dose as directed.
Itching
As the graft sites begin to heal and form crusts, itching is common, particularly at night when there are fewer distractions. Do not scratch the recipient area under any circumstances. The saline spray can provide temporary relief by moistening the crusts and soothing the skin. Some patients also find that a cool, damp cloth gently pressed against the non-grafted areas of the scalp provides relief.
Anxiety About Graft Safety
Many patients report that the psychological stress of worrying about their grafts keeps them awake. This is entirely normal. Remind yourself that as long as you are sleeping on your back at an elevated angle and nothing is pressing directly on the recipient zone, your grafts are safe. The grafts are placed inside tiny incisions and are held in by a combination of natural tissue tension and dried blood. They are more secure than most patients realize.
"In twenty-plus years of performing hair transplants, the patients who have the smoothest recoveries are the ones who prepare their sleeping setup before surgery day. Buying a wedge pillow or setting up a recliner in advance removes one more source of stress from the recovery process."
Sleeping Timeline Summary
| Period | Sleeping Position | Elevation | Side Sleeping |
|---|---|---|---|
| Nights 1-3 | Back only | 45 degrees | Not allowed |
| Nights 4-7 | Back only | 30 degrees | Not recommended |
| Nights 8-14 | Back preferred; side possible with care | 15-20 degrees | Allowed for frontal transplants (ask surgeon) |
| After 14 nights | Any position | Flat is fine | Fully allowed |
What to Buy Before Your Surgery
Preparation is the key to comfortable post-operative sleep. We recommend purchasing or arranging the following items before your procedure date so that everything is ready when you arrive home:
- Wedge pillow (30-45 degree angle): Available online or at home goods stores for approximately 30 to 60 dollars. Choose one that supports from the lower back to the head.
- U-shaped travel pillow: A memory foam version provides the best support and neck stabilization. Avoid inflatable versions, which can deflate overnight.
- Satin or silk pillowcase: Smooth fabric reduces friction against the scalp and is less likely to catch on scabs than cotton or linen.
- Two body pillows or large bed pillows: For side barriers to prevent rolling.
- Absorbent towel or waterproof pillow protector: To catch any oozing or saline spray residue during the first two nights.
- Saline spray and medications within arm's reach: Place everything on the nightstand so you do not need to get up and risk bumping the grafts in the dark.
Returning to Exercise and Activity
Once you can sleep normally, you are also approaching the point where you can begin reintroducing physical activity into your routine. The sleeping restrictions and activity restrictions follow a similar timeline because both are governed by the graft stabilization process. For specific guidance on when and how to safely resume exercise, see our article on exercise after a hair transplant.
The Bottom Line
Sleeping after a hair transplant requires some adjustment, but it is a temporary inconvenience that lasts only about two weeks. The combination of elevated back sleeping, the right pillow setup, and simple anti-roll strategies will protect your grafts through their most vulnerable period. Most patients report that by the end of the first week, they have adapted well to the new sleeping arrangement, and by day 14 they are back to their normal habits without any lasting disruption.
If you have concerns about sleeping after your procedure or want to discuss the best recovery plan for your specific situation, our team at Bellevue Hair Doctor is always available to answer your questions. A well-prepared patient is a comfortable patient, and a comfortable patient heals optimally.
Related Articles

Post-Op Care: The Critical First 48 Hours After Hair Transplant
Everything you need to do in the first two days after surgery to protect your grafts and set the stage for optimal healing.

Managing Swelling After a Hair Transplant
Effective strategies for reducing and managing post-operative swelling in the forehead and eye area after hair restoration surgery.

Hair Transplant Recovery Timeline: What to Expect Week by Week
A detailed week-by-week breakdown of the hair transplant healing process, from day one through full results at 12-18 months.
Schedule Your Free Consultation
Have questions about your recovery or considering a hair transplant? Our board-certified specialists are here to help.